Lab-grown ‘mini-guts’ could change how we treat Crohn’s disease

Cambridge scientists have grown ‘mini-guts’ in the lab to help understand Crohn’s disease, showing that ‘switches’ that modify DNA in gut cells play an important role in the disease and how it presents in patients. These could in future be used to identify the best treatment for an individual patient, allowing for more precise and personalised treatments.
Crohn’s disease is a form of inflammatory bowel disease (IBD). It is a life-long condition characterised by inflammation of the digestive tract that affects around one in 350 people in the UK, with one in four presenting before the age of 18. Even at its mildest, it can cause symptoms that have a major impact on quality of life including stomach pain, diarrhoea, weight loss and fatigue, but it can also lead to extensive surgery, inpatient admissions, exposure to toxic drugs and have a major impact on patient and their families.
While there is some evidence that an individual is at greater risk of developing the condition if a first-degree relative has Crohn’s, there has been only limited success in identifying genetic risk factors. As a result, it’s estimated that only 10% of inheritance is due to variations in our DNA.
Matthias Zilbauer, Professor of Paediatric Gastroenterology at the University of Cambridge and Cambridge University Hospitals NHS Foundation Trust (CUH), said: "The number of cases of Crohn’s disease and IBD are rising dramatically worldwide, particularly amongst younger children, but despite decades of research, no one knows what causes it.
"Part of the problem is that it’s been difficult to model the disease. We’ve had to rely mainly on studies in mice, but these are limited in what they can tell us about the disease in people."
In research published today in Gut, Professor Zilbauer and colleagues used cells from inflamed guts, donated by 160 patients, mainly patients and adolescents, at CUH to grow more than 300 mini-guts – known as organoids – in the lab to help them better understand the condition. Samples were donated by patients with Crohn’s disease and ulcerative colitis, as well as by patients unaffected by IBD.
"The organoids that we've generated are primarily from children and adolescents," said Professor Zilbauer. "They’ve essentially given us pieces of their bowel to help with our research. Crohn’s can be a severe condition to have to deal with at any age."
"Without our volunteers’ bravery and support, we would not be able to make such discoveries as this."
Professor Matthias Zilbauer
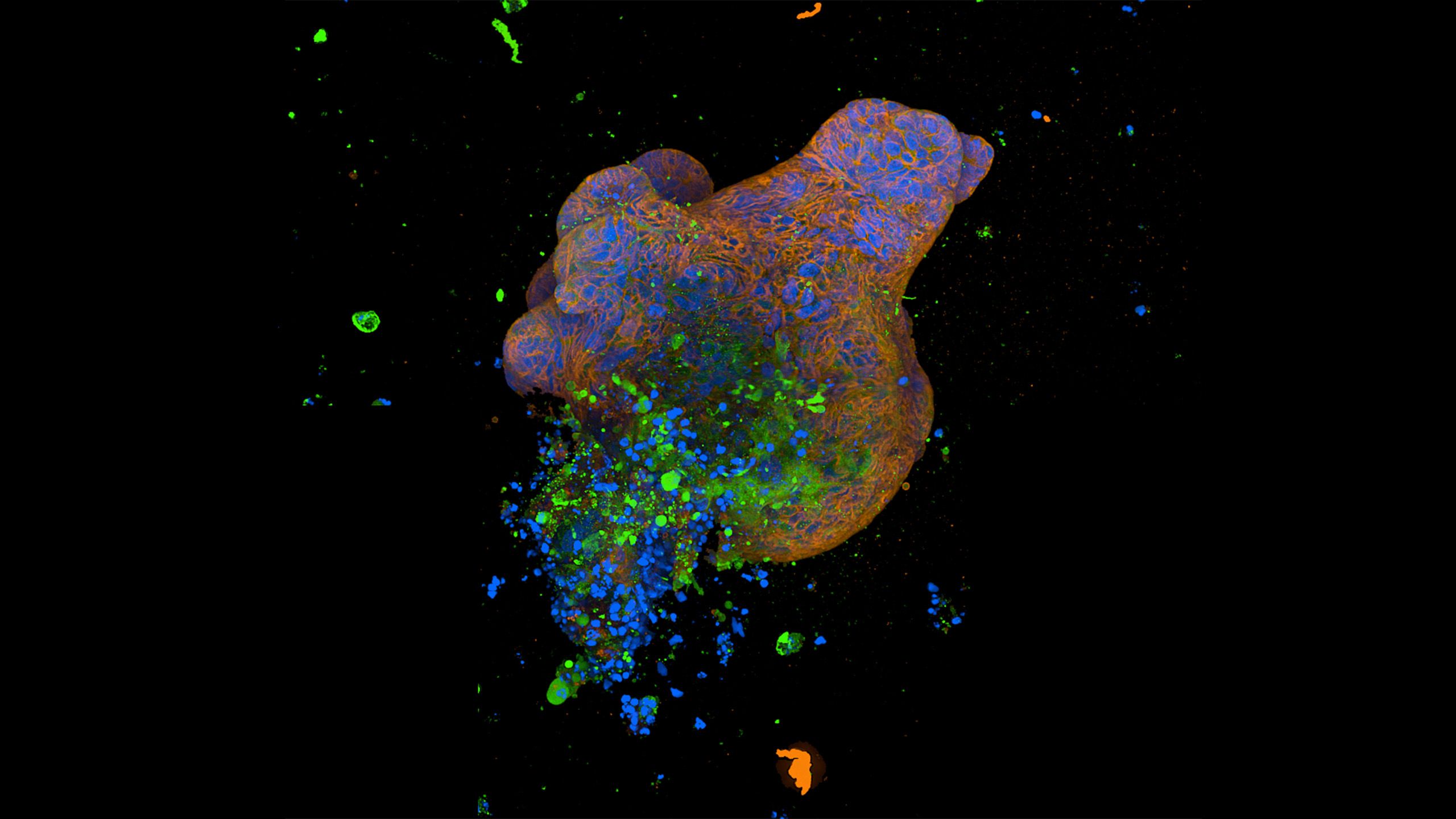
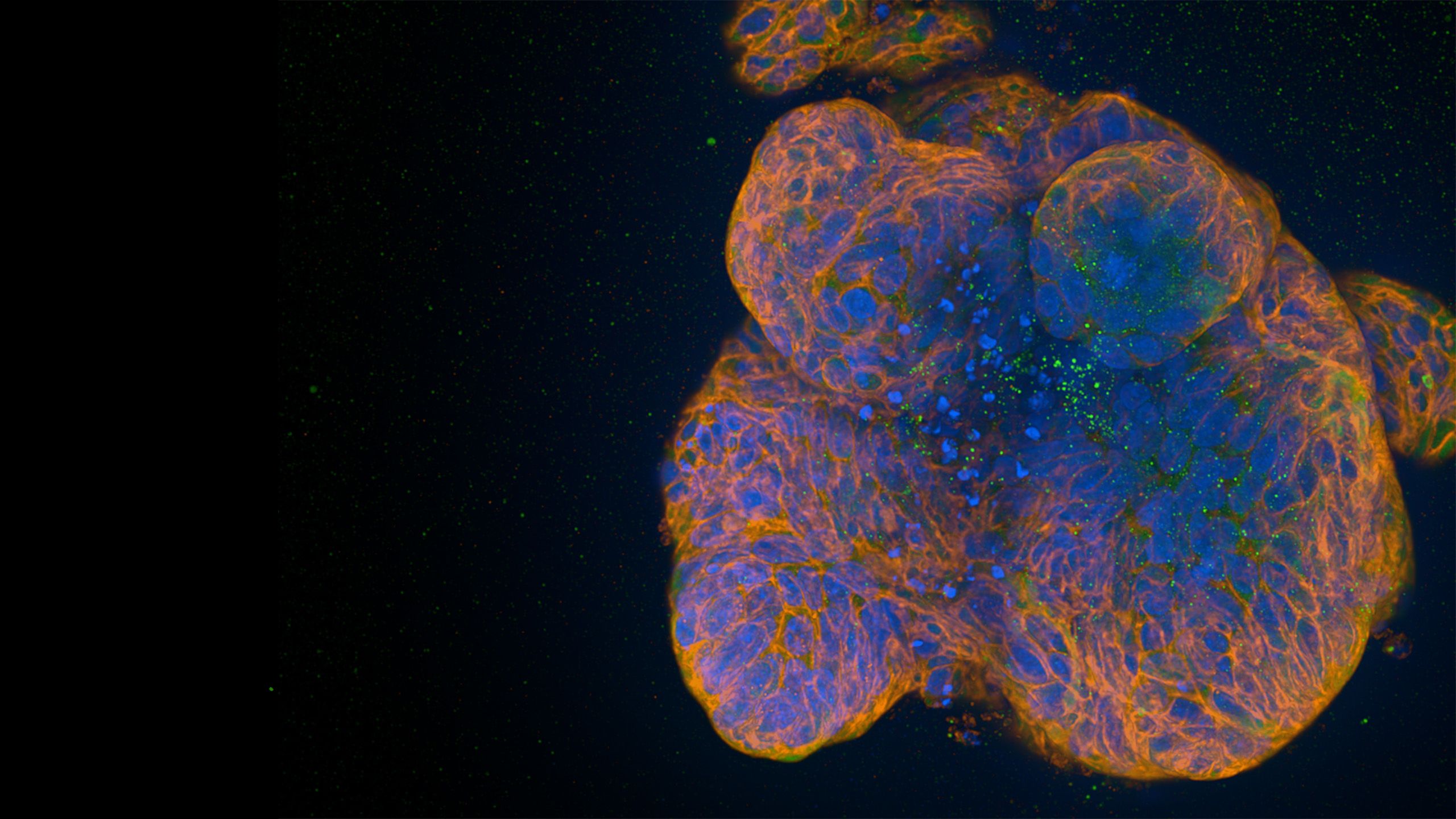
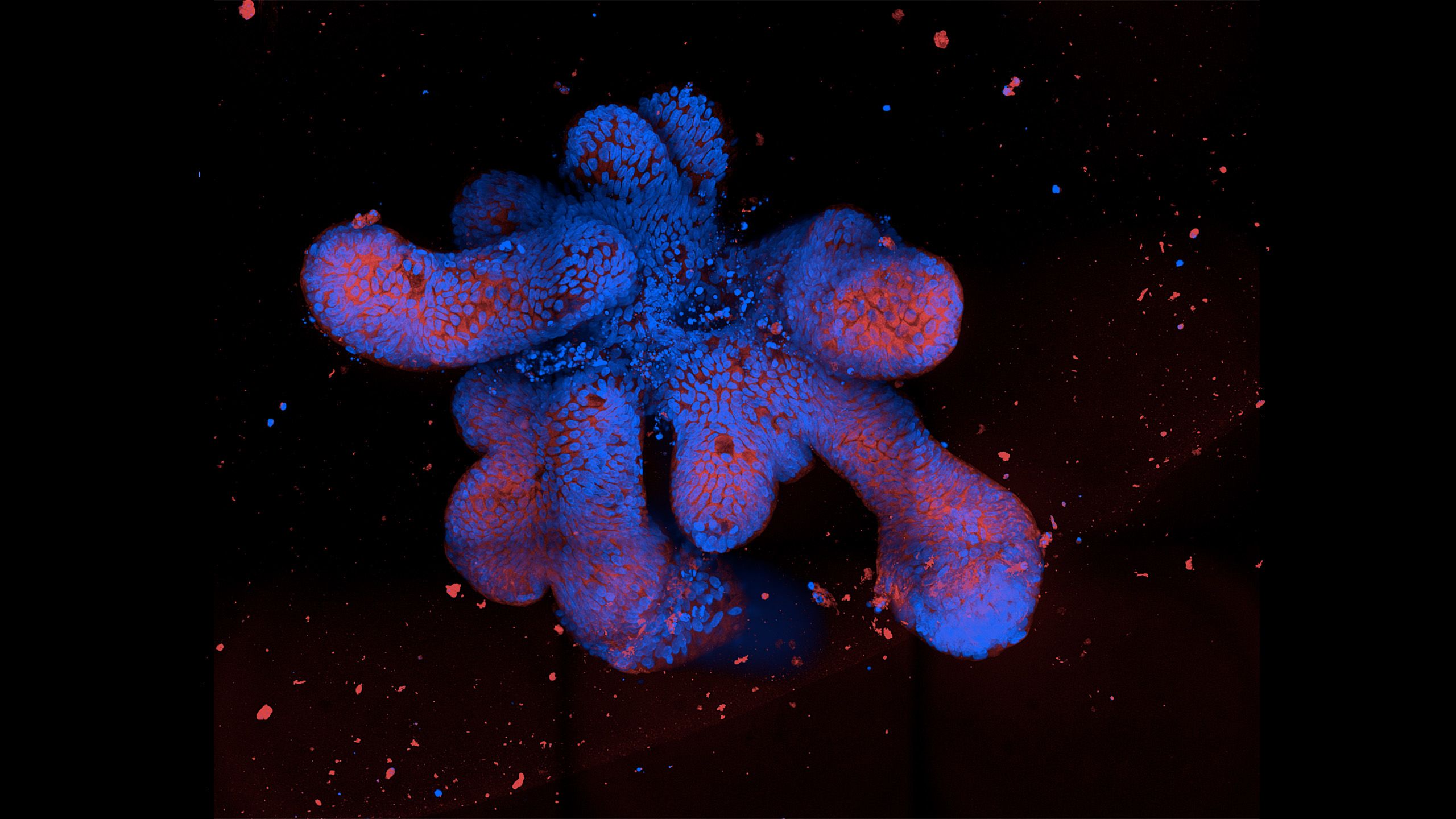
Organoids are 3D cell cultures that mimic key functions of a particular organ, in this case the epithelium – the lining of the gut. The researchers grew them from specific cells, known as stem cells, taken from the gut. Stem cells live forever in the gut, constantly dividing allowing the gut epithelium to regenerate.
Using these organoids, they showed that the epithelia in the guts of Crohn’s disease patients have different ‘epigenetic’ patterns on their DNA compared to those from healthy controls. Epigenetics is where our DNA is modified by ‘switches’ attached to our DNA that turn genes on and off – or turn their activity up or down – leaving the DNA itself intact, but changing the way a cell functions.
Professor Zilbauer, a researcher at the Stem Cell Institute at the University of Cambridge, said: "What we saw was that not only were the epigenetic changes different in Crohn’s disease, but there was a correlation between these changes and the severity of the disease. Every patient’s disease course is different, and these changes help explain why – i.e. not every organoid had the same epigenetic changes."
The researchers say the organoids could be used to develop and test new treatments, to see how effective they are on the lining of the gut in Crohn’s disease. It also opens up the possibility of tailoring treatments to individual patients.
Co-author Dr Robert Heuschkel, Consultant Paediatric Gastroenterologist at CUH and Lead of the Paediatric IBD Service, said: "At the moment, we have no way of knowing which treatment will work best for a patient. Even those treatments we currently have only work in around half of our patients and become less effective over time. It's a huge problem."
"In future, you could imagine taking cells from a particular patient, growing their organoid, testing different drugs on the organoid, and saying, ‘OK, this is the drug that works for this person’."
Dr Robert Heuschkel
The research highlighted a specific pathway implicated in Crohn’s, known as major histocompatibility complex (MHC)-I. This pathway allows immune cells to recognise antigens – that is, a toxin or other foreign substance that induces an immune response in the body, and which could include molecules in our food, or our gut microbiota. The team showed that the cells forming the inner lining of the gut in Crohn’s disease patients have an increased activity of MHC-I, which can lead to inflammation in specific parts of the gut.
"This is the first time where anyone has been able to show that stable epigenetic changes can explain what is wrong in the gut epithelium in patients with Crohn's disease," said Professor Zilbauer.
The epigenetic modifications were found to be very stable, which may explain why even after treatment, when a patient appears to be healed, their inflammation can return after several months – the drugs are treating the symptoms, not the underlying cause.
Epigenetic changes are programmed into our cells very early on during the development of the baby in the womb. They are influenced by environmental factors, which may include exposure to infections or antibiotics – or even lack of exposure to infection, the so-called ‘hygiene hypothesis’ that says we are not exposed to sufficient microbes for our immune systems to properly develop. The researchers say this may offer one possible explanation for how the epigenetic changes that lead to Crohn’s disease occur in the first place.
Arthur’s story: “It's quite cool to be part of the study”
Arthur Hatt has just returned from school. It’s been a particularly fun day today as rehearsals are underway for his school play, Aladdin – and he has one of its most important parts, the Genie.
Although Arthur is back at school full time now, there have been long periods where he was only able to manage half days. "I’d go in for the morning and then come home and just go to bed and sleep or read in bed," he says.
The reason is that Arthur has Crohn’s disease, a type of inflammatory bowel disease (IBD). Now aged 11, he was diagnosed with the condition aged nine – but his mother Sian says that in hindsight, he was showing symptoms from a very early age.
"From the age of about 12 to 18 months, he was having problems with his tummy – loose stools all the time and lots of stomach pains," she says.
Getting a diagnosis was not straightforward. There was no family history of inflammatory bowel disease or Crohn's disease, so no one thought to consider this option. (Since then, however, Arthur’s older brother has also been diagnosed with the condition.)
"We were told he had toddler diarrhoea, which is common and he’d probably grow out of," Sian says. "Then they said try eliminating dairy from his diet as it could be an intolerance. Then they said, oh, well, now try and eliminate gluten. When he was five or six, we got a referral to our local hospital who diagnosed him with abdominal migraines."
Eventually, Arthur was seen by a doctor who recognised the signs of IBD and gave him a simple test known as a faecal calprotectin test, which looks for unusually high levels of the protein calprotectin in the stools – a sign of inflammation. By this time, he was experiencing a lot of pain, as well as blood in his stools.
Following the test, he was referred to Addenbrooke’s Hospital, where he was seen by Professor Matthias Zilbauer.
"That was the first time really that we felt like, OK, somebody knows what's happening and there are things that they can do," says Sian.
Arthur was prescribed the drug azathioprine, which he is still on to this day. Because it can take time for the effects of the medication to work, he was also temporarily prescribed steroids. "They made me feel jittery," he says, "and I was really, really hungry."
Azathioprine by itself has not been enough to fully control his symptoms, so he has had to try several other medications. He is also receiving infliximab, which is given via infusion at Addenbrooke’s.
"The first indications seem to be quite promising," says Sian. "Even after the first dose, there seems to have been an improvement."
The drugs do, however, come with side-effects. Azathioprine, for example, can make the skin more sensitive to light, so Arthur has to wear sunscreen whenever he goes outside. The treatments also tend to suppress the immune system, leaving him more susceptible to infections.
"Autumn has been tricky in the past, because it's cough and cold and virus season at school," Sian says, "Arthur tends to pick up every one of them, and it's tiring for him when that happens."
The family have learned to pace themselves, working out through trial and error how much Arthur is able to do without tiring himself out.
"School holidays now are a lot more about resting than they are about busy days," Sian says. "We try and keep things quite chilled. He's so good at pushing through and doing things. He likes to be a busy bee, but we found that if he pushes through too much, he can then cause himself more trouble in the long run."
Fortunately, Arthur still manages to do the things he enjoys. He enjoys performing – hence his starring role in Aladdin. "I really like dancing, especially Latin and street dance," he says. "I manage to do most of the things I like, but I get tired sometimes."
Arthur is one of the children taking part in the Translational Research in Intestinal Physiology and Pathology (TRIPP) study at the University of Cambridge, which is aimed at understanding our gut health. He has donated some of the cells from his intestine, which Professor Zilbauer are colleagues are now using to grow ‘mini-guts’ to better understand Crohn’s disease. Arthur and his family have met the scientists at a family day at the hospital aimed at showing the children how they’re helping research.
"I think it's quite cool to be part of the study," he says. "It’s nice to know they're trying to get more information about Crohn’s."
Sian adds: "The real hope is that eventually, we’ll be able to take away a lot of the trial and error with what works and what doesn't work – because it’s different for every patient. That would be amazing."
These days, more and more children are being diagnosed with Crohn’s disease and IBD. To these children, Arthur has a message:
"There are bad days and there are good days, but eventually you'll find the right medicine. Sometimes it can take a really long time, but eventually they’ll find the thing that works for you."
For now, though, he’s just looking forward to getting on stage and working his magic on the audience.

Arthur Hatt, aged 11
Arthur Hatt, aged 11

The research was largely supported by the Medical Research Council. It was also supported through collaboration with the Milner Therapeutics Institute, University of Cambridge.
Cambridge Enterprise is working with Professor Zilbauer and team and has recently filed a patent for this technology. They are seeking commercial partners to help with the development of this opportunity.
Reference
Dennison, T et al. Patient-derived organoid biobank identifies epigenetic dysregulation of intestinal epithelial MHC-I as a novel mechanism in severe Crohn’s disease. Gut; 11 Jun 2024; 10.1136/gutjnl-2024-332043
Images
Immunofluorescence spinning disc microscopy images of organoids. (Thomas Dennison/ University of Cambridge)
The text in this work is licensed under a Creative Commons Attribution 4.0 International License